9 Alarming Truths About Celiac Disease: Powerful Nursing Strategies for Early Detection & Lifelong Care

Introduction
Celiac disease is a serious, lifelong autoimmune disorder that affects the digestive system and overall health. Despite growing awareness, thousands of people remain undiagnosed because the symptoms of celiac disease often mimic other gastrointestinal or systemic conditions.
For nurses and healthcare professionals, understanding celiac disease is not optional — it is essential. Early recognition can prevent long-term complications such as malnutrition, infertility, osteoporosis, neurological disorders, and even certain cancers.
This comprehensive guide explores celiac disease in depth — including its causes, pathophysiology, symptoms, diagnostic criteria, treatment, nursing interventions, complications, and patient education strategies — all structured to meet SEO standards aligned with Google Search Console recommendations.
What is Celiac Disease?
Celiac disease is a chronic autoimmune disorder triggered by gluten consumption. Gluten is a protein found in wheat, barley, and rye.
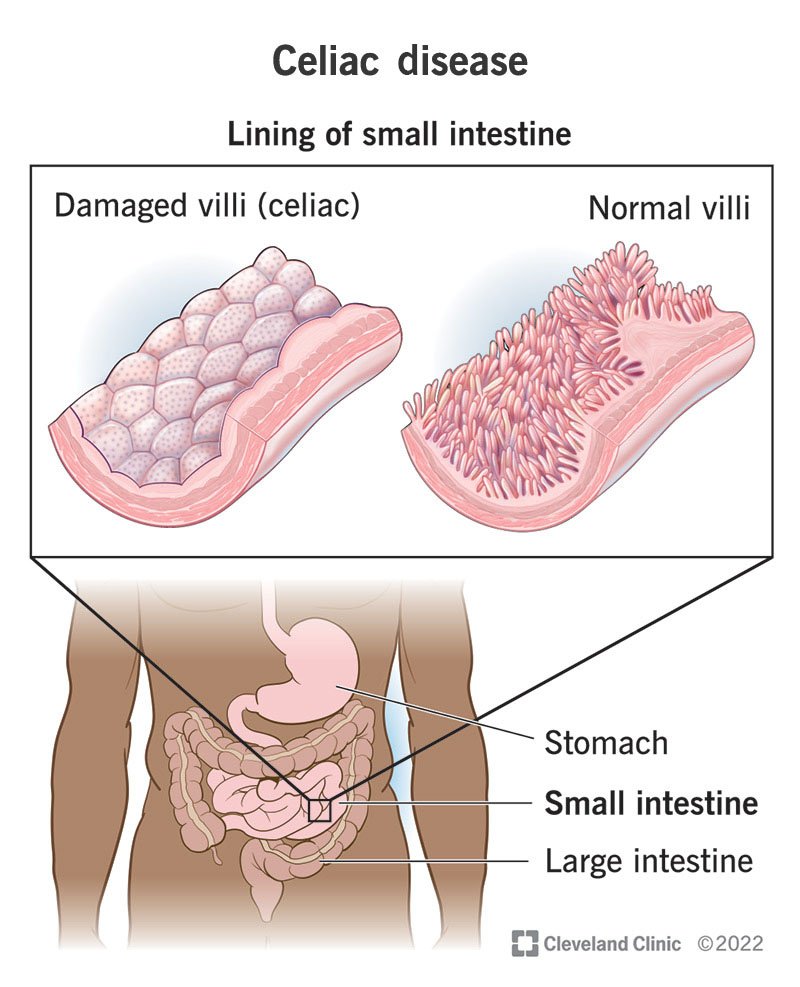
When individuals with celiac disease ingest gluten, their immune system mistakenly attacks the lining of the small intestine. Specifically, the immune response damages the villi — small finger-like projections responsible for nutrient absorption.
As villi become flattened or destroyed, the body cannot properly absorb nutrients. This leads to:
- Iron deficiency anemia
- Vitamin D deficiency
- Calcium deficiency
- Protein-energy malnutrition
- Weight loss or growth delay in children
Unlike simple food intolerance, celiac disease causes measurable intestinal damage and systemic complications.
Pathophysiology of Celiac Disease
Understanding the mechanism of celiac disease helps nurses explain it to patients effectively.
- Gluten enters the small intestine.
- Tissue transglutaminase (tTG) modifies gluten peptides.
- Immune cells recognize these peptides as harmful.
- Inflammatory cytokines are released.
- Villi become inflamed and flattened.
- Nutrient absorption decreases.
This autoimmune cascade continues as long as gluten is consumed.
Causes of Celiac Disease
Celiac disease develops due to a combination of genetic, environmental, and immune factors.
1. Genetic Predisposition
Most patients carry HLA-DQ2 or HLA-DQ8 genes. However, not everyone with these genes develops celiac disease.
2. Gluten Exposure
Gluten acts as the environmental trigger.
3. Immune Dysfunction
An abnormal immune response leads to self-tissue damage.
Family history significantly increases risk.
Risk Factors of Celiac Disease
- First-degree relative with celiac disease
- Type 1 diabetes
- Autoimmune thyroid disease
- Down syndrome
- Turner syndrome
- Selective IgA deficiency
Screening high-risk groups improves early detection rates.
Signs and Symptoms of Celiac Disease
Celiac disease presents with a wide range of symptoms.
Gastrointestinal Symptoms
- Chronic diarrhea
- Constipation
- Abdominal bloating
- Flatulence
- Nausea
- Vomiting
- Steatorrhea
Extraintestinal Symptoms
- Fatigue
- Iron-deficiency anemia
- Osteoporosis
- Peripheral neuropathy
- Depression
- Delayed puberty
- Infertility
Dermatological Manifestation
Dermatitis herpetiformis is a blistering skin rash strongly associated with celiac disease.
Children may present differently than adults, often with growth failure or irritability.
Diagnostic Criteria of Celiac Disease
Accurate diagnosis requires proper evaluation.
1. Serological Testing
- Anti-tTG IgA (first-line test)
- Endomysial antibodies (EMA)
- Total IgA level
2. Small Intestinal Biopsy
Gold standard confirmation showing villous atrophy.
3. Genetic Testing
Used when diagnosis remains uncertain.
Important: Patients must be on a gluten-containing diet before testing.
Complications of Untreated Celiac Disease
- Failure to treat celiac disease may lead to:
- Severe malnutrition
- Osteoporosis and fractures
- Reproductive problems
- Neurological disorders
- Small intestinal lymphoma
- Increased mortality risk
- Early treatment dramatically reduces complications.
Treatment of Celiac Disease
Currently, there is no cure for celiac disease.
The only proven treatment is:
Lifelong Strict Gluten-Free Diet
Avoid:
- Wheat
- Barley
- Rye
- Processed foods containing hidden gluten
Safe Foods:
- Rice
- Corn
- Quinoa
- Buckwheat
- Fruits and vegetables
- Lean meats
- Dairy (if tolerated)
- Nutritional Supplementation
- Patients may require:
- Iron
- Vitamin B12
- Calcium
- Vitamin D
- Folate
Dietitian referral is highly recommended.
Nursing Management of Celiac Disease
For readers of Empower Nursing Skill, nursing care plays a pivotal role.
1. Assessment
- Evaluate gastrointestinal symptoms
- Monitor weight and BMI
- Review lab results
2. Education
- Teach gluten-free label reading
- Explain cross-contamination risks
- Reinforce lifelong adherence
3. Emotional Support
- Address anxiety about eating out
- Encourage support groups
4. Monitoring
- Follow-up serology tests
- Assess symptom improvement
- Monitor bone health
5. Prevention of Complications
- Encourage DEXA scan for osteoporosis
- Promote vaccination updates
-
1. Is celiac disease the same as gluten sensitivity?
No. Celiac disease is an autoimmune disorder causing intestinal damage, while gluten sensitivity does not cause villous atrophy.
-
2. Can celiac disease develop in adulthood?
Yes. It can develop at any age.
-
Question3. Is celiac disease curable?
No, but it is completely manageable with a gluten-free diet.
-
4. How long does recovery take? Symptoms may improve within weeks, but full
Symptoms may improve within weeks, but full healing may take months or years.
-
5. Can children outgrow celiac disease?
No. It is a lifelong condition.



