Atrial Fibrillation: Symptoms, Causes & Treatment Guide

What is Atrial Fibrillation?
Atrial fibrillation is an irregular heartbeat, or arrhythmia. Atrial fibrillation also known as AFib or AF, caused by chaotic electrical signals in the heart’s upper chambers (atria), can lead to blood clots, stroke, heart failure and other heart-related complications. AFib is the most common type of irregular heart rhythm.

Description: Irregular and often rapid heart rhythm originating in the atria.
Characteristics: ECG Rhythm with absence of distinct P-waves, irregular R-R intervals.
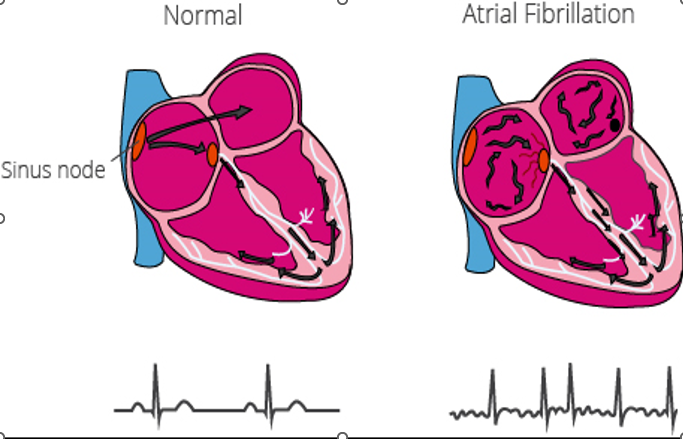
Normal Heart Rhythm vs Atrial Fibrillation
A NORMAL HEART RHYTHM is a coordinated heartbeat (60–100 bpm) initiated by the SA node,
while Atrial Fibrillation (AFib) is a chaotic, irregular, and often rapid arrhythmia originating from multiple sites in the atria, causing them to quiver.
Pathophysiology of Atrial Fibrillation
- Rapid and disorganized electrical activity occurs in the atria
- Electrical impulses originate from ectopic foci (pulmonary veins) instead of the SA node
- Leads to ineffective atrial contraction (atria quiver, not pump properly)
- Results in reduced cardiac output
- AV node receives chaotic signals and transmits them irregularly
- Causes irregularly irregular ventricular rhythm
- Ineffective contraction leads to blood stasis, especially in the left atrial appendage
- Increases risk of thrombus (clot) formation
- Clots may embolize → can cause stroke
- Long-term AF leads to atrial remodeling (dilation and fibrosis)
Four Main Types Of Atrial Fibrillation (Afib)
1. Paroxysmal AFib
- Episodes start suddenly and stop on their own
- Usually lasts less than 7 days (often < 24 hours)
- Heart returns to normal rhythm without treatment
- Symptoms may come and go (palpitations, dizziness)
2. Persistent AFib
- Lasts more than 7 days
- Does not stop on its own
- Requires treatment (medications or cardioversion) to restore normal rhythm
3. Long-Standing Persistent AFib
- Continuous AFib lasting more than 12 months
- Rhythm control becomes more difficult
- Often associated with structural changes in the atria
4. Permanent AFib
- AFib is accepted as ongoing
- No further attempts to restore normal rhythm
- Focus is on:
- Rate control
- Anticoagulation (to prevent stroke)
Clinical Symptoms of Atrial Fibrillation (AFib)
- Palpitations
- Fatigue Or Weakness
- Shortness Of Breath (Dyspnea)
- Dizziness
- Chest Pain Or Discomfort
- Reduced Exercise Capacity
- Fainting (Syncope
Diagnosis of Atrial Fibrillation (AFib)
- Electrocardiogram: Irregular rhythm and absence of P waves.
- Holter monitoring: 24–48 hours or longer.
- Echocardiography (2D Echo):Assesses heart structure, valve disease, and atrial enlargement.
- Chest X-ray : Helps evaluate heart size and lung conditions contributing to AFib.
- Blood tests : Includes thyroid function tests (TSH), electrolytes, and renal function.
Atrial Fibrillation (AFib) Management
- Control heart rate: Maintain a safe ventricular rate to improve cardiac output.
- Restore and maintain normal rhythm (sinus rhythm) :convert irregular rhythm to normal.
- Prevent thromboembolism (stroke prevention):Reduce risk of clot formation.
- Improve symptoms and quality of life: Reduce palpitations, fatigue, and breathlessness.
- Treat underlying causes:Manage conditions like hypertension, thyroid disorders, or heart disease.
Nursing Interventions
- Monitor vital signs (HR, BP, SpO₂) frequently.
- Assess ECG rhythm continuously.
- Symptom Assessment in which we evaluate for palpitations, chest discomfort, and shortness of breath.
- Administer prescribed medications (beta-blockers, calcium channel blockers, digoxin).
- INR Monitoring if the patient is on warfarin and heparin.
- Monitor for signs of bleeding (gums, urine, stool, bruising).
- Patient Position in semi-Fowler’s position to improve cardiac output.
- Monitor signs of reduced perfusion (fatigue, hypotension, altered mental status).
- Assess neurological status regularly (speech, limb strength, consciousness).
Pharmacological Management
- Anticoagulants: Prevent blood clot formation (e.g., warfarin, heparin, DOACs).
- Beta-blockers:Control heart rate (e.g., metoprolol, atenolol).
- Calcium channel blockers: Slow ventricular rate (e.g., diltiazem, verapamil).
- Antiarrhythmic drugs: Restore or maintain sinus rhythm (e.g., amiodarone, flecainide).
- Digoxin:Used for rate control, especially in heart failure patients.
Procedural & Surgical Interventions
- Electrical cardioversion – Controlled shock to restore normal heart rhythm.
- Catheter ablation – Destroys abnormal electrical pathways causing AFib.
- Pacemaker implantation – Used in patients with slow heart rate or post-ablation.
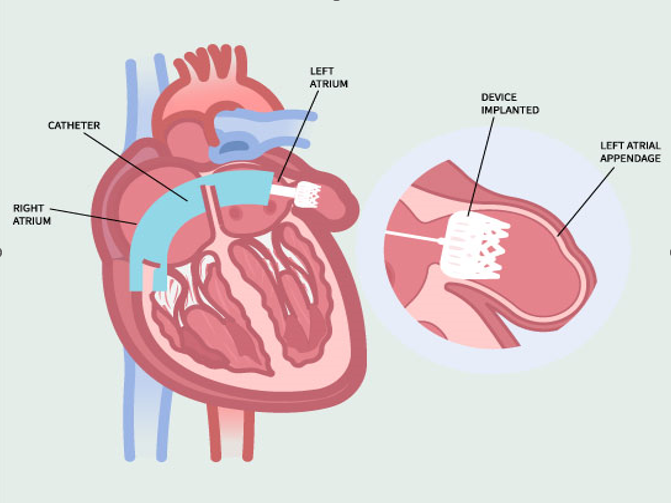
- Left atrial appendage closure (e.g., Watchman device) – Reduces stroke risk by preventing clot formation.
- Maze surgery – Creates scar tissue pathways to correct abnormal electrical signals.



